What is Nephrogenic Systemic Fibrosis (NSF)?
Nephrogenic systemic fibrosis (NSF), is a rare systemic fibrotic disorder that primarily involves the skin and subcutaneous tissues, but it can also affect other organs including the lungs, pleura, pericardium, skeletal muscle, and internal organs. It occurs in patients with severe acute or chronic renal dysfunction, including patients who are receiving dialysis of any form, and in many cases is believed to be secondary to the release of free gadolinium (Gd3+) ions from the chelates that constitute Gadoliniumbased contrast agents, with subsequent deposition of insoluble gadolinium phosphate precipitates in bodily tissues.
As the contrast agents are metabolized through the renal system, they have a prolonged half-life in patients with decreased renal function, increasing the likelihood that gadolinium release and deposition in tissues will occur. However, NSF can occur without exposure to gadolinium-based contrast agents.
When NSF is associated with gadolinium-based contrast agents, it usually manifests within 2 to 10 weeks following contrast administration. The risk of NSF may be related to the specific type of contrast agent, the cumulative dose, and the residual renal function of the patient. Macrocyclic gadolinium-based contrast agents are the most stable ones and are associated with the lowest risk of NSF, followed by linear ionic and linear nonionic agents in order of decreasing stability and associated increased risk of NSF.
Nephrogenic systemic fibrosis (NSF), has a high morbidity and mortality rate and has no known uniformly effective treatment. Therefore, patients who are planning to undergo MRI with gadolinium-based contrast agents must be carefully screened for renal dysfunction. When the estimated glomerular filtration rate (eGFR) is ≥60 mL/min/1.73m2, gadolinium-based contrast material can be administered as indicated, assuming there are no other contraindications. When the eGFR is 30 to 59 mL/min/1.73m2, a macrocyclic gadolinium-based contrast material can be administered using the lowest possible dose. When the eGFR is <30 mL/min/1.73m2, gadolinium-based contrast material is generally not administered unless there is an urgent medical necessity.

Symptoms Of Nephrogenic Systemic Fibrosis
The symptoms of Nephrogenic systemic fibrosis are:-
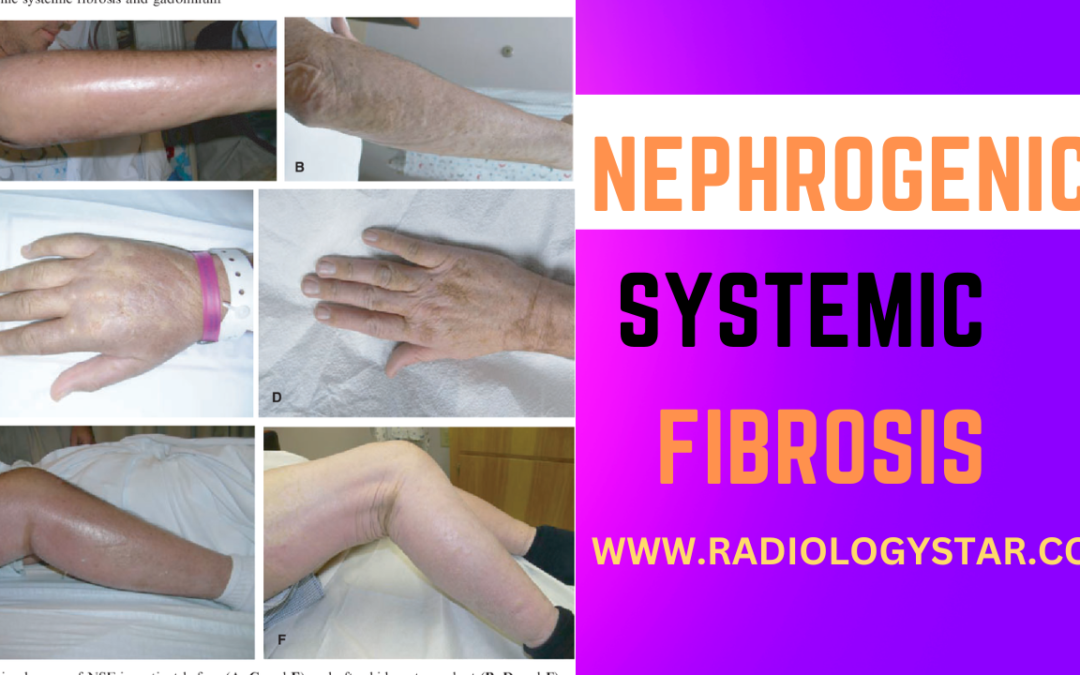
A. Skin thickening and hardening, which can limit mobility and flexibility.
B. Swelling of the extremities, often starting in the lower limbs and progressing upwards.
C. Red or dark patches on the skin.
D. Joint stiffness and pain.
E. Muscle weakness.
F. Systemic symptoms, such as fatigue, weakness, and muscle pain.
G. Burning, itching or severe sharp pains in areas of involvement.
H. Thickening and hardening of the skin, typically on the arms and legs and sometimes on the body, but almost never on the face or head
Causes Nephrogenic Systemic Fibrosis
The exact cause of nephrogenic systemic fibrosis (NSF) is not fully understood, but it has been strongly associated with the use of certain gadolinium-based contrast agents (GBCAs) in individuals with impaired kidney function. Here’s how it is believed to occur:-
A. Impaired Kidney Function:- Nephrogenic systemic fibrosis primarily affects individuals with impaired kidney function, particularly those with severe kidney disease (chronic kidney disease stage 4 or 5) or those on dialysis. In individuals with healthy kidneys, GBCAs used in contrast-enhanced imaging studies like magnetic resonance imaging (MRI) or magnetic resonance angiography (MRA) are typically cleared from the body quickly. However, when kidney function is compromised, the clearance of GBCAs is delayed, leading to their accumulation in the bloodstream.
B. Gadolinium Retention:- Gadolinium is a heavy metal used in some contrast agents to enhance the visibility of certain tissues in imaging studies. In Nephrogenic systemic fibrosis, it is believed that the retained gadolinium may play a role in triggering the condition. Gadolinium can be deposited in various tissues throughout the body, including the skin, leading to an abnormal response.
C. Fibrosis and Tissue Changes:- The retained gadolinium may trigger an abnormal fibrotic response in the connective tissues of the skin and other organs. This fibrosis results in the thickening, hardening, and tightening of the affected tissues, which are characteristic features of Nephrogenic systemic fibrosis.
It’s important to note that not all gadolinium-based contrast agents are associated with the same risk of NSF. The risk appears to be higher with certain types of linear GBCAs, particularly those containing gadodiamide and gadopentetate dimeglumine. Therefore, healthcare providers take precautions to minimize the use of high-risk GBCAs in individuals with kidney impairment.
Risk Factors For Nephrogenic Systemic Fibrosis.
The main risk factor for developing NSF is exposure to gadolinium-based contrast agents (GBCAs) used in medical imaging procedures like magnetic resonance imaging (MRI) or magnetic resonance angiography (MRA). Here are the key risk factors for NSF:-
A. Impaired Kidney Function:- The most significant risk factor for NSF is impaired kidney function. When the kidneys are not functioning properly, they may have difficulty clearing GBCAs from the bloodstream, leading to their accumulation and potential toxicity. Individuals with chronic kidney disease, especially those with severe kidney impairment, are at the highest risk.
B. Dialysis:- Patients undergoing dialysis have a higher risk of developing NSF because their kidneys are unable to efficiently filter out substances like gadolinium from the bloodstream. This increases the likelihood of gadolinium retention and the development of NSF.
C. Type of Gadolinium Contrast Agent:- The risk of NSF varies depending on the specific type of GBCA used. Some linear GBCAs, particularly those containing gadodiamide and gadopentetate dimeglumine, have been associated with a higher risk of NSF compared to macrocyclic GBCAs. Healthcare providers now take precautions to minimize the use of high-risk GBCAs in at-risk individuals.
D. Cumulative Gadolinium Exposure:- The risk of NSF may also be influenced by the cumulative exposure to GBCAs. Repeated or high-dose exposures to GBCAs can increase the likelihood of gadolinium retention and the development of NSF.
E. Recent GBCA Administration:- NSF typically occurs within a few weeks to months after the administration of a GBCA. Therefore, recent exposure to GBCAs, particularly high-risk ones, is a risk factor for NSF development.
FAQs.
Q. What is nephrogenic systemic fibrosis (NSF)?
NSF is a rare medical condition that primarily affects individuals with impaired kidney function. It is characterized by the hardening and thickening of the skin and connective tissues throughout the body.
Q. What causes NSF?
NSF is strongly associated with the use of certain gadolinium-based contrast agents (GBCAs) in individuals with impaired kidney function.
Q. What are the symptoms of NSF?
Symptoms include skin thickening, skin discoloration, swelling, joint stiffness and pain, limited mobility, and, in severe cases, internal organ involvement.
Q. Who is at risk of developing NSF?
Individuals with severe kidney disease (chronic kidney disease stage 4 or 5) or those on dialysis are at the highest risk. Cumulative exposure to GBCAs and the type of GBCA used also influence risk.
Q. What are the different types of GBCAs?
GBCAs are categorized as linear or macrocyclic. Linear GBCAs, like gadodiamide and gadopentetate dimeglumine, are associated with a higher risk of NSF.
Q. How is NSF diagnosed?
Diagnosis involves clinical evaluation, reviewing medical history, and sometimes skin biopsies to confirm the condition.
Q. Can NSF be prevented?
Healthcare providers take precautions to minimize the use of high-risk GBCAs in at-risk individuals, and guidelines have been developed to reduce the risk of NSF.
Q. Is there a cure for NSF?
There is no specific cure for NSF, but early detection and management can help minimize its impact.
Q. What is the treatment for NSF?
Treatment focuses on managing symptoms and may involve physical therapy, pain management, and interventions to improve mobility.
Q. Can NSF be fatal?
While NSF itself is not typically fatal, in severe cases, internal organ involvement can lead to life-threatening complications.
Q. Are there any long-term complications of NSF?
Long-term complications can include permanent skin and joint changes that may impact mobility and quality of life.
Q. Is NSF contagious?
No, NSF is not contagious. It is not caused by an infectious agent and cannot be transmitted to others.
Q. Is there ongoing research on NSF?
Yes, researchers continue to study NSF to better understand its causes and develop more effective treatments.
Q. Can NSF be mistaken for other skin conditions?
NSF can sometimes be mistaken for other skin conditions like scleroderma or eosinophilic fasciitis due to similar symptoms.
Q. Is there a genetic predisposition to NSF?
NSF is not known to have a strong genetic component. It primarily occurs in individuals with impaired kidney function.
Q. Can NSF spontaneously improve or resolve?
NSF tends to be a progressive condition, and spontaneous improvement or resolution is rare.
Q. Can individuals with NSF undergo MRI or MRA without contrast agents?
In some cases, alternative imaging methods that do not require contrast agents may be considered for individuals with NSF.
Q. Can NSF be prevented by using specific GBCAs?
Safer macrocyclic GBCAs are preferred for individuals at risk of NSF to reduce the likelihood of development.
Q. Should I be concerned about NSF if I have kidney disease?
If you have kidney disease and require contrast-enhanced imaging, discuss your risk with your healthcare provider and make informed decisions about the procedure.
Q. Is NSF still a concern in medical practice today?
NSF awareness and preventive measures have reduced the incidence of NSF, but it remains a concern, especially in individuals with impaired kidney function.
BOOK LINK :- Textbook of Radiology for X-ray, CT, MRI, BSc, BRIT and MSc Technicians